Esther Borges Florsheim
-
Phone: 480-727-3391
-
-
727 E Tyler Street Rm A330B The Biodesign Institute A Tempe, AZ 85287-7501
-
Mail code: 5701Campus: Tempe
-
Esther Borges Florsheim is an immunologist with a core interest in how immunological defenses promote fitness and organismal survival. She studies allergies, mast cell biology, and neuroimmune interactions in the gastrointestinal tract to determine the impact of the immune system on physiology and behavior.
Dr. Florsheim earned one degree in Fundamental Sciences for Health (B.Sc., University of São Paulo) and one in Immunology (Ph.D., University of São Paulo). Her interests in ideas from across immunology and inflammation have led her on a dedicated research trajectory, performing undergraduate research on innate inflammatory responses to bacterial lipopolysaccharides and focusing her graduate research on the innate immune pathways required for the development of allergies. She completed her postdoctoral training at Yale University School of Medicine where she explored how allergen sensing by the gastrointestinal immune system changes behavior.
As a Principal Investigator, Dr. Florsheim aims to: a) transform the immunology field through a multidisciplinary approach, b) motivate the next generation of scientists interested in discovering the yet unsolved immunological mysteries, and c) create an equal world in STEM.
2014 Ph.D. Immunology University of Sao Paulo
2009 B.Sc. Fundamental Sciences for Health University of Sao Paulo
Immunology is a rapidly growing area in the biomedical sciences and at the forefront of current research priorities. While progress in immunology has mostly emphasized defense strategies against pathogens, most of our knowledge on how immunological processes affect normal physiology remains poorly understood. The Florsheim Lab’s goal is to fill this gap and expand our understanding of the immune system as integral to the whole organism, uniting concepts from physiology, neuroscience, and animal behavior.
_______________________________ OUR PROJECTS ________________________________
We use a multi-disciplinary approach to redefine
the role of the immune system in health and disease.
___
I. Integrating mast cell biology and gastrointestinal physiology
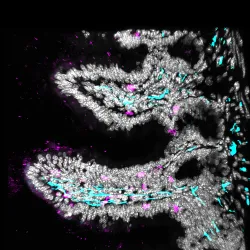
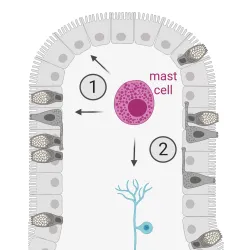
The gastrointestinal (GI) tract, where most of the immune cells in the body live, is the largest site of interaction with the environment. Resident cells such as macrophages, dendritic cells, and innate lymphoid cells are fundamental to maintaining the integrity and support this tissue demands. Mast cells are also endemic to the entire GI tract, but apart from their role in anaphylaxis, their contribution to gut physiology is unknown. Our group aims to determine how mast cells regulate GI physiology at a steady state and during inflammation (food allergy, for example). GI physiology includes digestion, motility, and secretory and endocrine functions. This research project provides new insights into the biology of mast cells as well as new therapeutic avenues to ameliorate inflammatory diseases of the GI tract.
II. Neuroimmune connections
The immune and nervous systems are the body’s main sensory interfaces that perceive and adapt to the environment. Despite the relevance of these two systems, immunology and neuroscience have been historically separate fields of study. It is well appreciated that immune cells (e.g. mast cells and innate lymphoid cells) form stable interactions with neurons to influence organismal physiology. Disruption of this module might be at the origin of inflammatory conditions. By leveraging technologies from these two biomedical fields, we seek to identify the cellular and molecular mechanisms of neuroimmune interactions at mucosal surfaces.
III. Brain circuits and behavioral outcomes
The best way to deal with allergies is to avoid exposure to allergens. This avoidance behavior is characteristic of allergy sufferers and essential for animals to prevent exposure to noxious substances in natural environments. Despite its significance, the mechanisms by which inflammation causes behavioral changes are mostly unknown. The Florsheim lab designs experiments to a) identify the brain circuits induced by immune defenses and b) dissect the behavioral responses to distinct immunological stimuli. Our approach has the potential to uncover unknown immunological mechanisms underlying neuropsychiatric conditions, such as anxiety, depression, and post-traumatic stress disorder.
________________________________ LAB MISSION ________________________________
The Florsheim Lab welcomes scientists from underrepresented backgrounds. As a team,
we are committed to providing a diverse, inclusive, and supportive environment. We work
together to help the next generation of scientists by focusing on career development,
scientific integrity, and the pursuit of fundamental biological questions.
Postdoctoral Researcher
- Ana Cristina Roginski
Graduate students - PhD
- Pooja Kher
- Bruna Costa Lima
- Cheyanne Woodrow
Undergraduate students
- Leslie Bustamante Hernandez
- Fathima Nawaz
- Brandon Lazna
Alumni
- Jahnvi Parmar (undergraduate student)
- Mayka Galarza (undergraduate and 4+1 MS)
- Fernando Arcos Juan (undergraduate student and research technician)
- Rebecca Reinking-Herd (Biology MS student)
Highlighted publications
- Florsheim EB*#, Bachtel ND*, Cullen J, Costa Lima BG, Godazgar M, Carvalho F, Chatain C, Zimmer M, Zhang C, Gautier G, Launay P, Wang A, Dietrich MO, and Medzhitov R#. Immune sensing of food allergens promotes avoidance behaviour. Nature (2023). https://doi.org/10.1038/s41586-023-06362-4. * co-authors, #corresponding authors.
We reported how allergen sensing by immune cells in the gastrointestinal tract changes animal behavior. We suggest that lipid mediators called cysteinyl leukotrienes produced by mast cells upon allergen exposure drive changes in the central nervous system to induce avoidance.
- Florsheim EB*, Sullivan ZA*, Khoury-Hanold W*, Medzhitov R. Food allergy as a biological food quality control system. Cell, 2020. * co-authors. Review
In this review article, we discuss food allergies from a broader physiological perspective, providing a unique framework to understand the origins of these mysterious diseases.
- Florsheim E, Yu S, Bragatto I, Faustino L, Gomes E, Ramos RN, Barbuto JA, Medzhitov R, Russo M. Integrated innate mechanisms involved in airway allergic inflammation to the serine protease subtilisin. J Immunol, 2015.
This work characterized allergic responses to the occupational allergen subtilisin, a bacterial serine protease, and detailed the main innate immune pathways underlying subtilisin sensitization. Subtilisin revealed potent adjuvant properties to unrelated bystander antigens, suggesting that exposure to allergens with intrinsic activity (such as proteases) increases the risk to develop allergies to unrelated environmental proteins, which is likely the case for many known allergies.
- Palm NW, Rosenstein RK, Yu S, Schenten DD, Florsheim E, Medzhitov R. Bee venom phospholipase A2 induces a primary type 2 response that is dependent on the receptor ST2 and confers protective immunity. Immunity, 2013.
We found that IgE induced by repeated exposures to bee venom PLA2 can protect mice from future challenges with a near-lethal dose of PLA2. This was one of the first findings suggesting that allergies can be beneficial when not excessive and suggests that allergic defenses might play a physiological role.
- Mirotti L, Florsheim E, Rundqvist L, Larsson G, Spinozzi F, Leite-de-Moraes M, Russo M, Alcocer M. Lipids are required for the development of Brazil nut allergy: the role of mouse and human iNKT cells. Allergy, 2013.
In this work, we identified the allergenic activity of lipids in the development of nut allergy. Our data showed that lipids could function as adjuvants to induce allergic responses and the mechanism involved the activation of iNKT cells.
Courses
2025 Summer
| Course Number | Course Title |
|---|---|
| BIO 495 | Undergraduate Research |
| BIO 495 | Undergraduate Research |
2025 Spring
| Course Number | Course Title |
|---|---|
| BIO 493 | Honors Thesis |
| BIO 494 | Special Topics |
| BIO 494 | Special Topics |
| MBB 495 | Undergraduate Research |
| BIO 495 | Undergraduate Research |
| MIC 420 | Immun: Molecular&Cell Foundtns |
| BIO 420 | Immun: Molecular&Cell Foundtns |
| MIC 598 | Special Topics |
| MCB 598 | Special Topics |
| BIO 420 | Immun: Molecular&Cell Foundtns |
| MIC 420 | Immun: Molecular&Cell Foundtns |
| BIO 420 | Immun: Molecular&Cell Foundtns |
| MIC 420 | Immun: Molecular&Cell Foundtns |
2024 Fall
| Course Number | Course Title |
|---|---|
| BIO 492 | Honors Directed Study |
| BIO 495 | Undergraduate Research |
| MBB 495 | Undergraduate Research |
| BIO 598 | Special Topics |
| LIA 194 | Special Topics |
| BIO 498 | Pro-Seminar |
2024 Summer
| Course Number | Course Title |
|---|---|
| BIO 495 | Undergraduate Research |
| BIO 495 | Undergraduate Research |
2024 Spring
| Course Number | Course Title |
|---|---|
| BIO 493 | Honors Thesis |
| BIO 494 | Special Topics |
| MBB 495 | Undergraduate Research |
| BIO 495 | Undergraduate Research |
| MIC 420 | Immun: Molecular&Cell Foundtns |
| BIO 420 | Immun: Molecular&Cell Foundtns |
| MIC 598 | Special Topics |
| MCB 598 | Special Topics |
| BIO 420 | Immun: Molecular&Cell Foundtns |
| MIC 420 | Immun: Molecular&Cell Foundtns |
| BIO 420 | Immun: Molecular&Cell Foundtns |
| MIC 420 | Immun: Molecular&Cell Foundtns |
2023 Fall
| Course Number | Course Title |
|---|---|
| BIO 492 | Honors Directed Study |
| BIO 495 | Undergraduate Research |
| MBB 495 | Undergraduate Research |
| BIO 598 | Special Topics |
| BIO 498 | Pro-Seminar |
2023 Summer
| Course Number | Course Title |
|---|---|
| BIO 495 | Undergraduate Research |
| BIO 495 | Undergraduate Research |
2023 Spring
| Course Number | Course Title |
|---|---|
| BIO 493 | Honors Thesis |
| BIO 494 | Special Topics |
| BIO 495 | Undergraduate Research |
| MIC 420 | Immun: Molecular&Cell Foundtns |
| BIO 420 | Immun: Molecular&Cell Foundtns |
| MIC 598 | Special Topics |
| MCB 598 | Special Topics |
2022 Fall
| Course Number | Course Title |
|---|---|
| BIO 492 | Honors Directed Study |
| BIO 495 | Undergraduate Research |
| MBB 495 | Undergraduate Research |
2022 Summer
| Course Number | Course Title |
|---|---|
| BIO 495 | Undergraduate Research |
| BIO 495 | Undergraduate Research |
2022 Spring
| Course Number | Course Title |
|---|---|
| BIO 493 | Honors Thesis |
| BIO 494 | Special Topics |
| BIO 495 | Undergraduate Research |
| MIC 420 | Immun: Molecular&Cell Foundtns |
| BIO 420 | Immun: Molecular&Cell Foundtns |
| MIC 598 | Special Topics |
| MCB 598 | Special Topics |
| MIC 420 | Immun: Molecular&Cell Foundtns |
| BIO 420 | Immun: Molecular&Cell Foundtns |
2021 Fall
| Course Number | Course Title |
|---|---|
| BIO 492 | Honors Directed Study |
| BIO 493 | Honors Thesis |
| BIO 495 | Undergraduate Research |
| NEU 591 | Seminar |
| BIO 498 | Pro-Seminar |
| BIO 598 | Special Topics |
2021 Summer
| Course Number | Course Title |
|---|---|
| BIO 495 | Undergraduate Research |
| BIO 495 | Undergraduate Research |
2021 Spring
| Course Number | Course Title |
|---|---|
| BIO 495 | Undergraduate Research |
The Society for Advancement of Chicanos/Hispanics and Native Americans in Science (SACNAS), member (2024 - present)
The American Association of Immunologists, member (2021 - present)
PsychoNeuroImmunology Research Society, member (2020 - 2024)
The Brazilian Society for Immunology, member (2006 - 2012)
Graduate programs (2021 - present):
- Molecular and Cellular Biology, MS and PhD
- Neuroscience, PhD
- Biology, MS
Ad hoc reviewer
Immunity, The Journal of Clinical Investigation, eLife, Frontiers in Immunology, Nature Communications, The Journal of Immunology, PLOS One, The International Journal of Molecular Sciences, Mediators of Inflammation, Biomedical Journal.